Insulin dosing often gets reduced to a search term, but in practice it is a care pathway. A safe plan for basal insulin includes a starting dose, a slow titration schedule, glucose monitoring, and a clear route back to the prescriber when readings change.
That wider system matters. Some patients use services such as CanadianInsulin, a prescription referral platform. Where required, it helps confirm prescription details with the prescriber, while dispensing and fulfilment are handled by licensed third-party pharmacies, where permitted. Some patients also explore cash-pay options and cross-border fulfilment depending on eligibility and jurisdiction.
Why Basal Insulin Dosing Starts Conservatively
Basal insulin covers the body’s background insulin need between meals and overnight. For insulin glargine U-100, often known by the brand Lantus, the effect is designed to be steady rather than rapid.
The first dose is rarely chosen to normalize every reading at once. If the starting dose is too high, the main danger is hypoglycemia, especially overnight. If it is too low, high fasting glucose may persist, but that is usually safer to correct in steps.
People often search for a single brand-name dose, but the larger question is how clinicians balance control against risk. The answer depends on diabetes type, body size, age, kidney function, other medicines, and whether low glucose has happened before.
How Clinicians Choose A Starting Dose
For many adults with type 2 diabetes, basal insulin is started at 10 units once daily or about 0.1 to 0.2 units per kilogram per day. Those are common starting points, not fixed rules. A clinician may start lower in older adults, in people with kidney disease, or when the risk of low glucose is high.
Type 1 diabetes is different. Basal insulin is only one part of a full regimen that also includes mealtime insulin. In that setting, clinicians usually estimate a total daily insulin need first, then assign a portion of that to basal coverage.
Before writing the first dose, prescribers usually review several variables:
- fasting glucose patterns and A1C
- body weight and recent weight change
- kidney and liver function
- use of steroids or other medicines that raise glucose
- meal timing, alcohol intake, and shift work
- past episodes of severe or unrecognized hypoglycemia
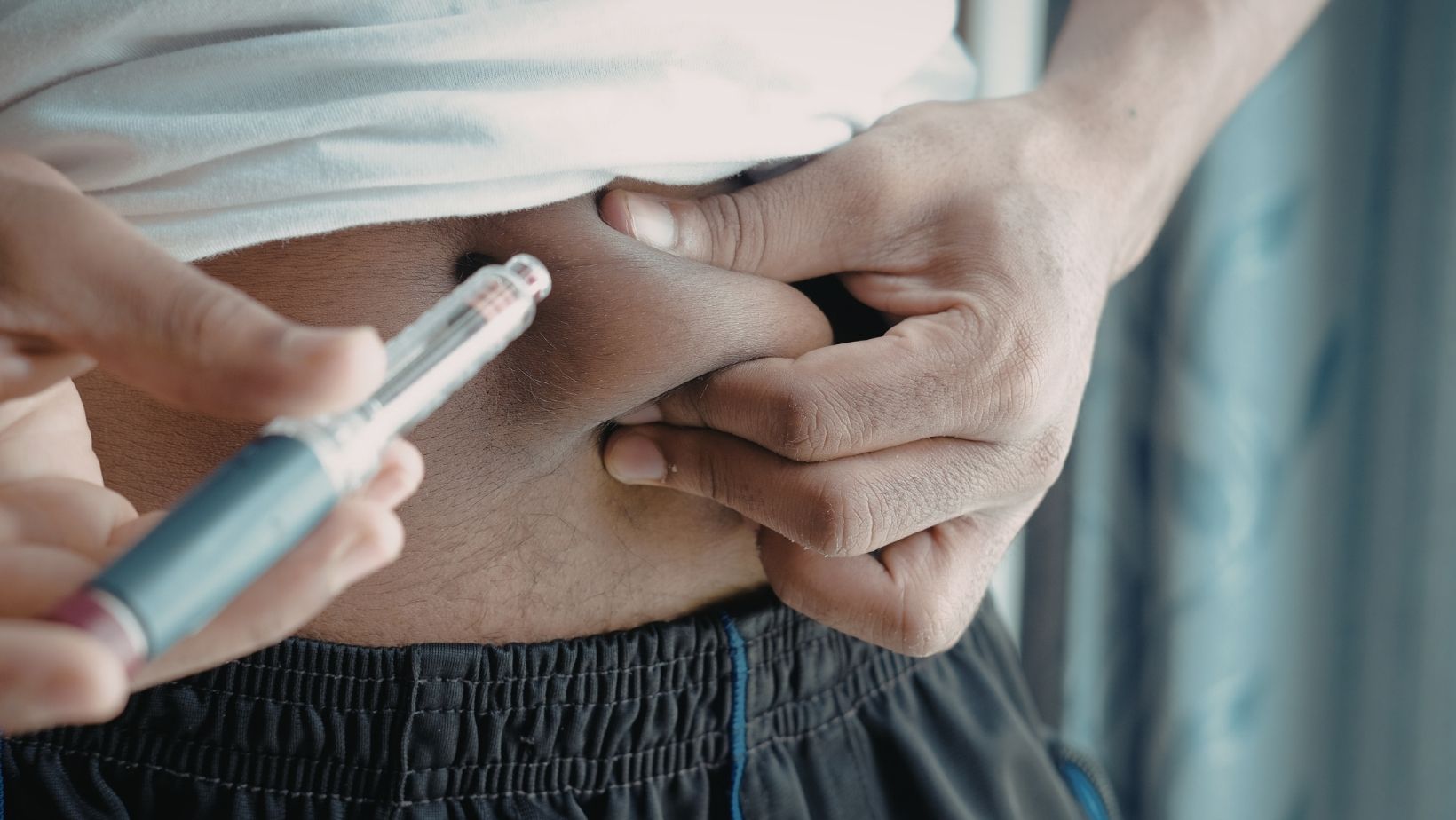
Injection technique also matters. A correct dose can still look ineffective if insulin is injected into scarred tissue, stored improperly, or taken at inconsistent times.
What Titration Usually Looks Like
Titration means adjusting the dose in small steps after the start. Most plans use fasting glucose as the main signal, because basal insulin mainly affects overnight and between-meal levels.
In type 2 diabetes, many clinicians increase the dose every three to four days, or once a week, if fasting readings remain above target and no lows occur. A common adjustment is 2 units at a time or about 10 to 15 percent, but the exact schedule varies by regimen and by the clinician’s instructions.
The reverse also matters. If fasting readings are low, or if a person wakes with sweating, confusion, headache, or shakiness, the dose may need to come down. Persistent morning highs do not always mean basal insulin should go up; late meals, missed mealtime insulin, illness, or the dawn phenomenon can all change the pattern.
Long-acting insulin should not be used as a quick correction for a single high reading unless the prescriber has given that instruction. Some practices give patients a written self-titration plan, while others prefer dose changes only after a call or portal message. Brand-specific directions can vary, as noted in this background on long-acting insulin dosing, but the safety principle is the same: adjust with a plan, not by guesswork.
When A Stable Dose May Need Analysis
A dose that worked last month may not fit current circumstances. Insulin needs often change during infection, after steroid treatment, with major shifts in diet or activity, or after weight loss.
Kidney disease can reduce insulin clearance and increase the risk of hypoglycemia. Reduced appetite, skipped meals, or increased alcohol use can do the same. On the other side, steroids, stress, poor sleep, and some acute illnesses can push glucose higher.
Clinicians also look for signs that the dose is trying to solve the wrong problem. If glucose is high after dinner but normal overnight, pushing basal insulin higher may only raise the risk of lows before breakfast. That is one reason insulin adjustment works best when it uses several days of glucose data, not a single reading.
Why Follow-Up Matters As Much As The Prescription
Starting insulin safely depends on more than the number on the pen. People need a target range, a schedule for checking glucose, and instructions for what counts as a low reading. They also need to know when to seek urgent help, especially if severe hypoglycemia, vomiting, dehydration, or very high glucose develops.
Care systems handle the practical side in different ways. Some patients work only through their local clinic and pharmacy. Others navigate insurers, telehealth, or referral platforms that help verify prescription details while licensed third-party pharmacies handle dispensing and fulfilment where permitted.
That distinction matters because access logistics and clinical decision-making are not the same task. A prescriber sets the regimen. Safe titration depends on medical follow-up, accurate glucose records, and a clear plan for dose changes when the clinical picture shifts.
The Broader Takeaway
Basal insulin is usually started low and adjusted slowly. For many adults with type 2 diabetes, common starting doses are modest, while people with type 1 diabetes usually need a fuller regimen review before a basal dose is set. In both cases, titration is guided by fasting glucose trends and by the risk of low blood sugar.
No single number is right for every adult, and the safest plan is individual rather than formula-driven.
Medical disclaimer: This content is for informational purposes only and is not a substitute for professional medical advice.

